“Nipple thrush pain is often described as burning, itching, or stinging and may be mild to severe. The pain is usually ongoing and doesn’t go away with improved positioning and attachment of your baby to the breast.”
“When you have nipple thrush, your nipple appearance may change to being shiny in appearance, sometimes chapped, blistered with white patches but may also look completely normal. You may also experience itchy, flaky and red nipples or areola.”
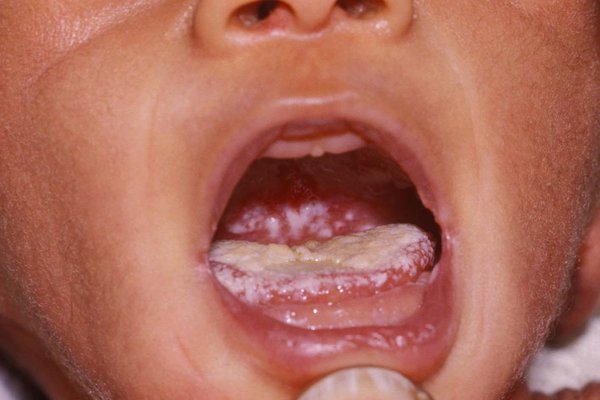
Thrush is an overgrowth of candida or yeast. It mostly commonly causes an infection and overgrowth in people who are immunocompromised. It can overgrow in areas with skin folds which are moist and warm, like armpits, the vagina, etc. It’s very rare to have yeast/candida/thrush in highly vascularized areas like the breasts and nipples.
Research has shown that in cases of suspected thrush the parent is most likely experiencing mastitis
“microbiological analysis of milk samples provided by 529 women with symptoms compatible with “mammary candidiasis”. Nipple swabs and nipple biopsy samples were also collected… Results showed that the role played by yeasts in breast and nipple pain is, if any, marginal…our results strongly support that coagulase-negative staphylococci and streptococci are the agents responsible for such cases.“
When providers visually assess for thrush, they may be seeing dermatitis rather than a yeast overgrowth on the nipples. Dermatitis is an allergic reaction or irritation caused by something the parent is sensitive to on their skin. This can include creams, ointments, and medications.
Here are some pictures of parents who thought they had thrush but actually had dermatitis!
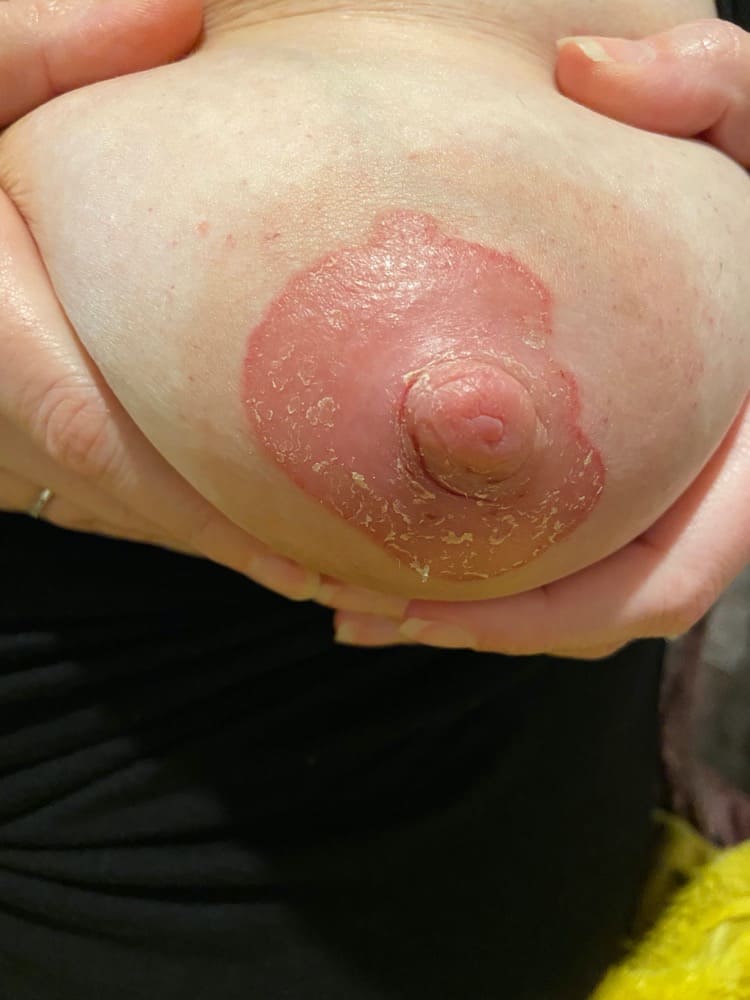
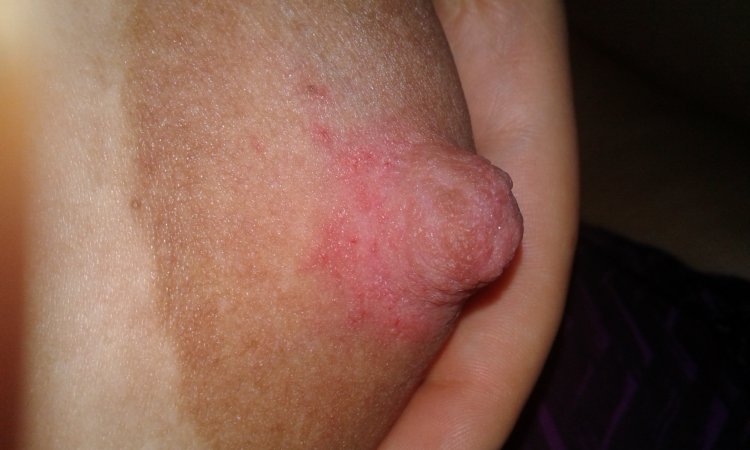
Below, is what yeast on the skin actually looks like
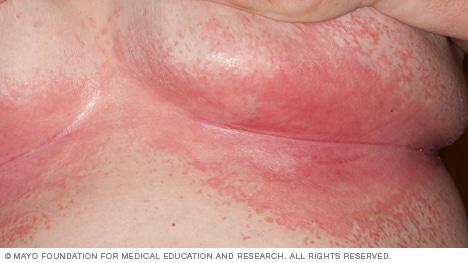
So what you should you do if you think you have thrush?
Talk to your Lactation Consultant for a full feeding and breast evaluation. They can make referrals to providers for treatment, if needed, and can help figure out what’s actually going on!
❤ Megan




