





❤ Megan








❤ Megan





We’ve talked about how PCOS and insulin resistance can affect lactation and milk production before but let’s explore this a bit more.

There is a disproportionate incidence of diabetes among ethnic groups.
Prevalence of diagnosed diabetes was highest among American Indians/Alaska Natives (14.7%), people of Hispanic origin (12.5%), and non-Hispanic blacks (11.7%), followed by non-Hispanic Asians (9.2%) and non-Hispanic whites (7.5%).
This, of course, is not the only disparity found in lactation among different ethnic groups.
However, insulin resistance plays an important role in the physiological barriers to successful feeding as well as the perception or expectation of failure.
PCOS is a syndrome and the combination of symptoms is unique in each case, making identification more challenging. Many people never receive a formal diagnosis.
Symptoms can include:
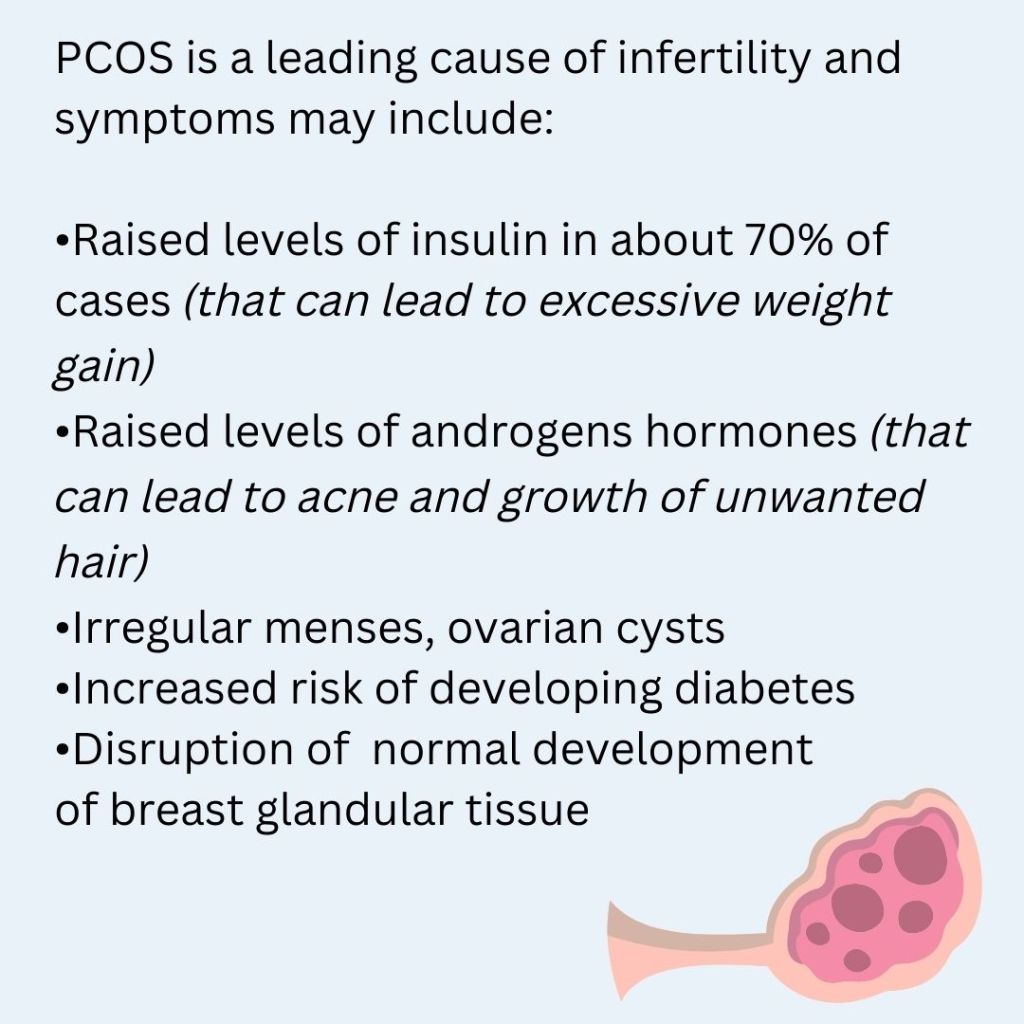
•Raised levels of insulin (that can lead to excessive weight gain)
•Raised levels of androgens hormones (that can lead to acne and growth of unwanted hair)
•Irregular menses, ovarian cysts
•Increased risk of developing diabetes
•Underdevelopment of breast glandular tissue – not size
Medical conditions related to insulin resistance create additional challenges to lactation. Insulin resistance may delay Lactogenesis II – which is the milk transition from colostrum to mature milk and copious volume increase – this may be delayed by up to a week.
Some people with IR may never make enough milk to meet all the needs of their infant because of the role insulin plays in milk production and glandular growth during pregnancy, however, we do not know in advance that a person with diabetes will have insufficient supply.
Our focus should be on best practices to support these parents in the optimal outcomes for milk production and healthy infant feeding. We can do this by supporting nutrition which does not focus on weight alone, through offering medication therapy if indicated during pregnancy, by increasing access to lactation care both in-patient and after discharge, and increasing access to human donor milk for supplementation.
As providers we can also learn more about non-medication supports for managing milk supply which can include:
• Frequent milk removal using hands-on techniques
• Learning about which herbs to use or avoid
• Avoiding pacifiers and bottles, instead focusing on skin-to-skin and using at breast supplement tools
• The use of donor milk until milk production is established
• Frequent visits with an IBCLC in the first week after delivery
• Supporting in-home care
• Using Peer Support programs to encourage parents and monitor the need for medical intervention
With support, education, and provider support parents with PCOS can chestfeed successfully!
❤ Megan
“Nipple thrush pain is often described as burning, itching, or stinging and may be mild to severe. The pain is usually ongoing and doesn’t go away with improved positioning and attachment of your baby to the breast.”
“When you have nipple thrush, your nipple appearance may change to being shiny in appearance, sometimes chapped, blistered with white patches but may also look completely normal. You may also experience itchy, flaky and red nipples or areola.”
Thrush is an overgrowth of candida or yeast. It mostly commonly causes an infection and overgrowth in people who are immunocompromised. It can overgrow in areas with skin folds which are moist and warm, like armpits, the vagina, etc. It’s very rare to have yeast/candida/thrush in highly vascularized areas like the breasts and nipples.
Research has shown that in cases of suspected thrush the parent is most likely experiencing mastitis
“microbiological analysis of milk samples provided by 529 women with symptoms compatible with “mammary candidiasis”. Nipple swabs and nipple biopsy samples were also collected… Results showed that the role played by yeasts in breast and nipple pain is, if any, marginal…our results strongly support that coagulase-negative staphylococci and streptococci are the agents responsible for such cases.“
When providers visually assess for thrush, they may be seeing dermatitis rather than a yeast overgrowth on the nipples. Dermatitis is an allergic reaction or irritation caused by something the parent is sensitive to on their skin. This can include creams, ointments, and medications.
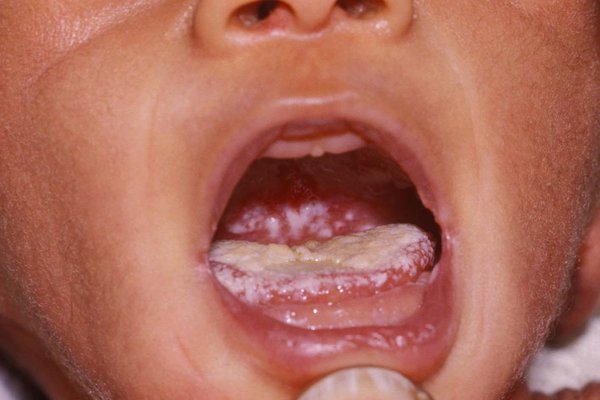
Here are some pictures of parents who thought they had thrush but actually had dermatitis!
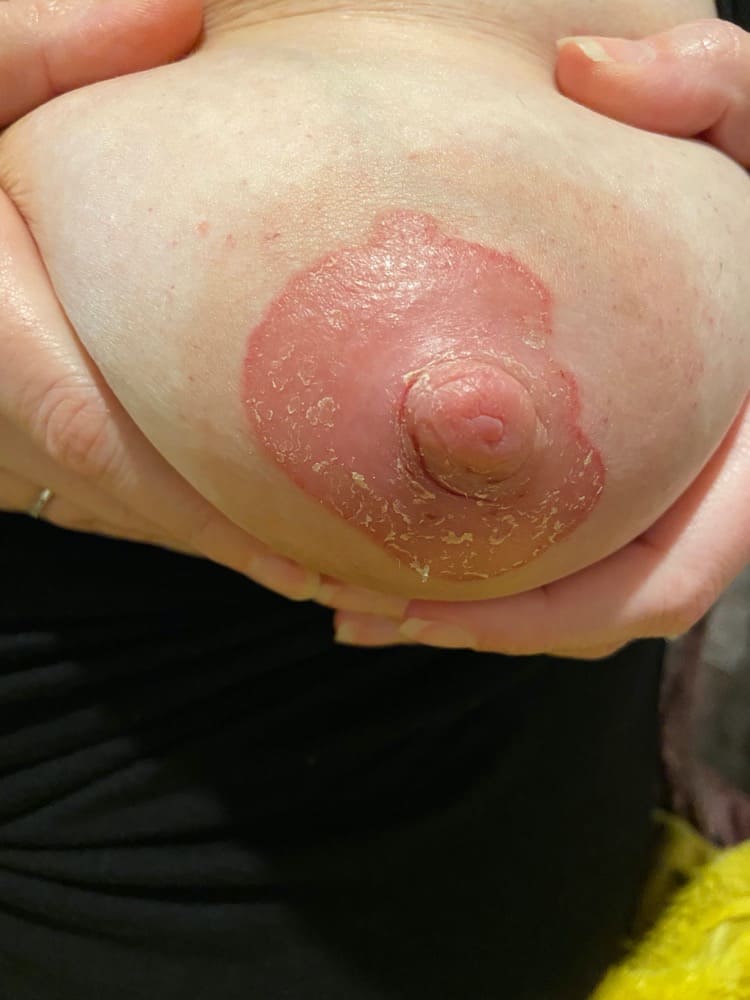
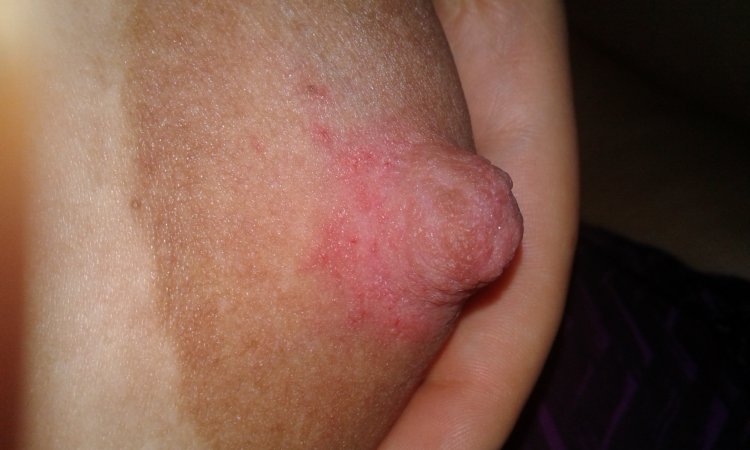
Below, is what yeast on the skin actually looks like
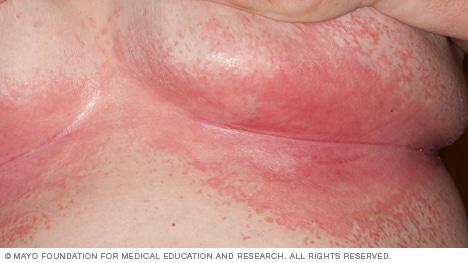
So what you should you do if you think you have thrush?
Talk to your Lactation Consultant for a full feeding and breast evaluation. They can make referrals to providers for treatment, if needed, and can help figure out what’s actually going on!
❤ Megan

Many people with diabetes and gestational diabetes meet their breastfeeding goals but others may experience challenges with their milk supply and/or delays in developing a full milk supply. Insulin is an essential hormone for full milk production and luckily there are many things we can do during pregnancy and postpartum to support our bodies and meet our breastfeeding goals.
Working with your Registered Dietitian and a Lactation Consultant as part of your health team is helpful for creating a plan that works well for your individual needs.
Nutritional Supports During Pregnancy and Postpartum:
Fiber! Oats are a really excellent source of fiber and they can help you feel full longer as well as stabilize your blood sugar. Try adding a handful into a morning protein smoothie. Your Dietician can share many other recipe ideas that might work for you. Quinoa is another great choice for protein and fiber!
B12 is a necessary vitamin that we get from animal sources. It gives us energy and maintains our nervous system. Getting adequate B12 from meat, fish, eggs, cheese, milk, and some fortified whole grain cereals throughout your pregnancy and postpartum period will support milk production.
Vitamin D is very important for lots of functions in our body. It supports our immune system, maintains healthy bones, and is supportive of our mood regulation. You’ll find it in milk, egg yolks, salmon, tuna, and in some fortified whole grain cereals. Be sure to get your recommended daily amount!
Calcium and Protein from dairy-free sources may be advised. Salmon, tofu, dark green leafy veggies, nut butters, and grass fed meat are good sources.
Other foods and herbs
Cumin – anti-diabetic, enhances mammary growth
Dill – works best with other herbs, supports insulin, diuretic (helps with swelling and engorgement)
Fennel – anti-androgenic, digestive support, diuretic
Myo-inositol – natural sugar found in citrus fruits, cantaloupe, and some beans which regulates blood sugars, can also be taken as a supplement
Herbs to support milk production
Each herb does a different job; there is no one size fits all. Below are some common herbs for insulin resistance shown to support milk production
Goat’s rue taken during the 3rd trimester and for the first 6 weeks can encourage glandular growth (the milk making cells). You can find it in drops called tinctures or in capsules. Vitex or Chasteberry is an herb commonly used for hormonal regulation. It can also be taken during pregnancy and postpartum.
Discuss the use of these herbs with your provider to determine which is right for your circumstances!
AVOID fenugreek. This herb is found in lots of lactation blends but it’s not an appropriate choice for people with diabetes as it affects your blood sugar and reduces the absorption of other oral medications.
Milk expression
If you are not at risk for preterm delivery, milk expression during pregnancy is a good idea. Not only does this stimulate for better long term milk production but you can freeze your colostrum and have it available after delivery if baby has hypoglycemia (low blood sugar). This decreases the chance that your baby will need donor milk or formula. Talk with your IBCLC about how to safely do this.
Megan Dunn, IBCLC