In honor of our Black parents, I’d like to share the following articles and resources:
The B.L.A.C.K. Course – A full-scope lactation and breastfeeding education course made by and for Black People and folks supporting Black breastfeeding.
Black History Month 2021 Toolkit
Melanated Mammary Atlas – The Melanated Mammary Atlas® is your portal to a world of images displaying mammary related conditions on Asian, Indigenous, Black and Brown folks.
Chocolate Milk: The Documentary – A film about the state of breastfeeding in Black America from The African American Breastfeeding Project.
Articles and blogs
THE HISTORY OF BLACK WOMEN & BREASTFEEDING
Breastfeeding As An Act Of Resistance For The Black Mother
Organizations Focused on Black Breastfeeding
African-American Breastfeeding Coalition of Oregon
Black Mothers’ Breastfeeding Association
Breastfeeding Sisters That Are Receiving Support (BSTARS)
Indiana Black Breastfeeding Association
National Association of Professional and Peer Lactation Supporters of Color (NAPPLSC)
Many medications are totally fine to take during lactation. Many meds won’t affect milk production and they won’t harm your baby!
Medications, prescription and over the counter, are processed through several steps which determine how much makes it into your milk and determines if it will affect your baby or the milk production process.
Let’s take a look at this process!
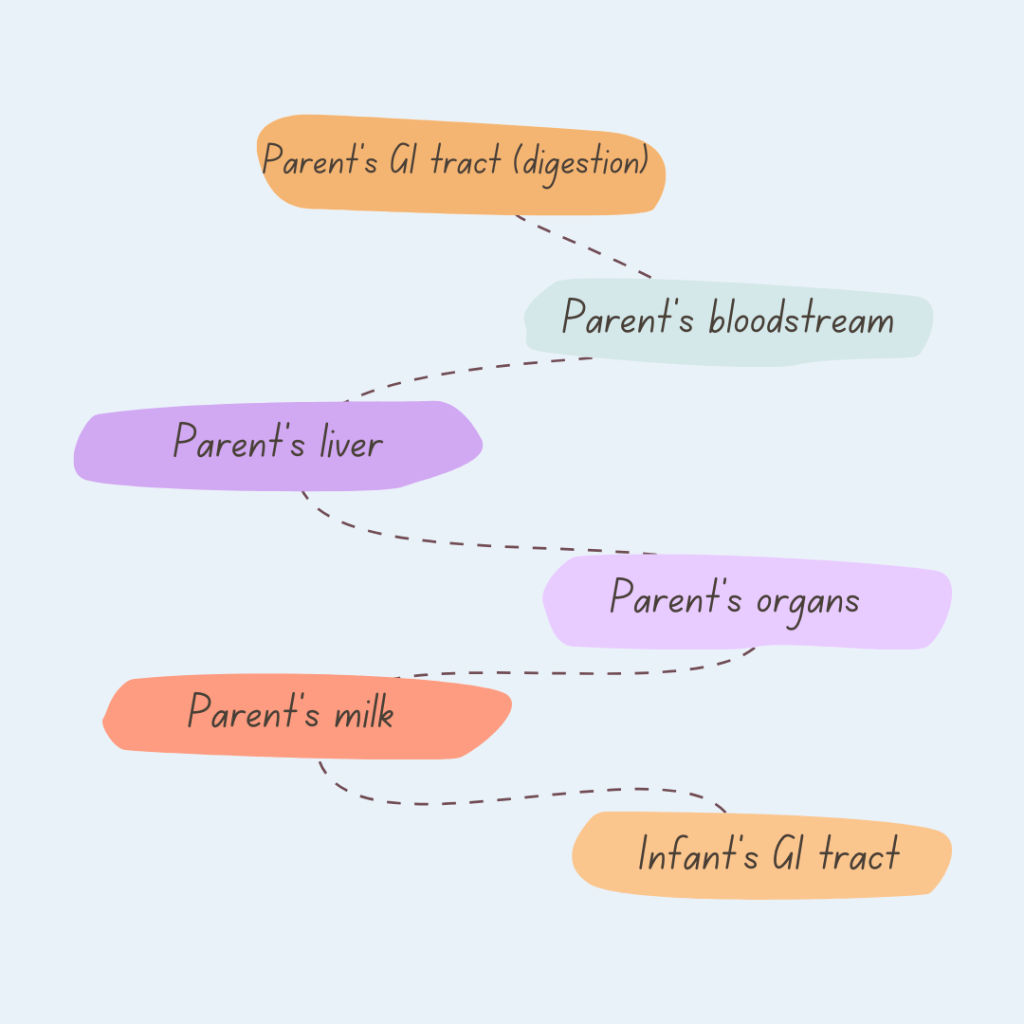
As you can see oral medications need to be digested, metabolized through the liver, processed through the target organs, before they can make it into the mammary tissue of the breast and into the milk.
If they make it that far the remaining molecules still have to be small enough and attracted to water, fat, or both to make it into the milk.
If it makes it into the milk it still needs to be digested and processed through baby’s liver before it will possibly affect baby!
Most medications are diluted to 0.5-10% of the parent’s dose before they even make it to baby! That’s very small!
There’s a lot that goes into determining if a medication is safe for you and baby during lactation. You can discuss the medications, supplements, and herbal remedies you are considering with your IBCLC who will provide you with resources to talk with your doctor.
Often there are alternatives if the medication you want to take is not compatible.
Since it’s cold and flu season you can check here for information about common medications you may be thinking of taking if you get symptoms.
The flu vaccine is safe to take while breastfeeding and gives your baby extra protection!
Life with a new baby is exciting and full of new experiences! But the holidays also bring chaos, lots of visits, travel, and stress. Which are the last things that new parents and babies need. When the holiday season rolls around, your family and friends will no doubt be thrilled to include your little one. How do you protect the peace and keep the boundaries for your family?
Here’s some ideas:
These conversations can be tough! Ask your partner and close friends to step in and help you navigate.
Bodywork or manual therapy includes many types of hands-on treatments focused on supporting normal movement and function.
This can include chiropractic care, cranial sacral therapy, osteopathic manipulation, and many other therapies!
When selecting a provider ask about them how often they care for infants and what additional training they have for working with babies.

Babies who experience a challenging birth – like a c-section, vacuum, or even just a not ideal position in the womb – often present with tension in their body which can impact their feeding, contentedness, sleep, and crying.
On the flip side, an infant with feeding problems can, over time, develop these same problems due to compensations.
What’s a compensation?
A compensation is what we do when the normal way of doing something isn’t working.
Twist your left ankle? Well, you might lean into using your right side a bit more until you heal.
It’s the same with our babies
If it’s not comfortable to move or feed in the normal way, they may develop compensations.
Okay, what’s the problem with that?
Compensations when used long term are dysfunctions.
Baby is using muscles which aren’t developed enough to work how they are using them. It also puts baby into a stressful state called sympathetic state.
This often means they cry more, have digestive problems are just generally not content. This is stressful for parents, too!
Bodywork and manual therapy for infants is incredibly gentle and works with their body to get back to balance. Gentle touch and massage can be beneficial for all babies!
And if your baby is having feeding problems which aren’t resolving with basic help or interventions, if your baby cries a lot, has sleep or nap difficulties, or it just doesn’t feel right…be sure to contact your provider and IBCLC for a referral to a skilled infant bodyworker. It may be just the thing your baby needs to feel better.
❤ Megan
This year in the Willamette Valley cases of respiratory illness among infants and children are skyrocketing. Many infants are experiencing illnesses which don’t usually peak until January.
You can protect your baby from RSV and other respiratory illnesses.
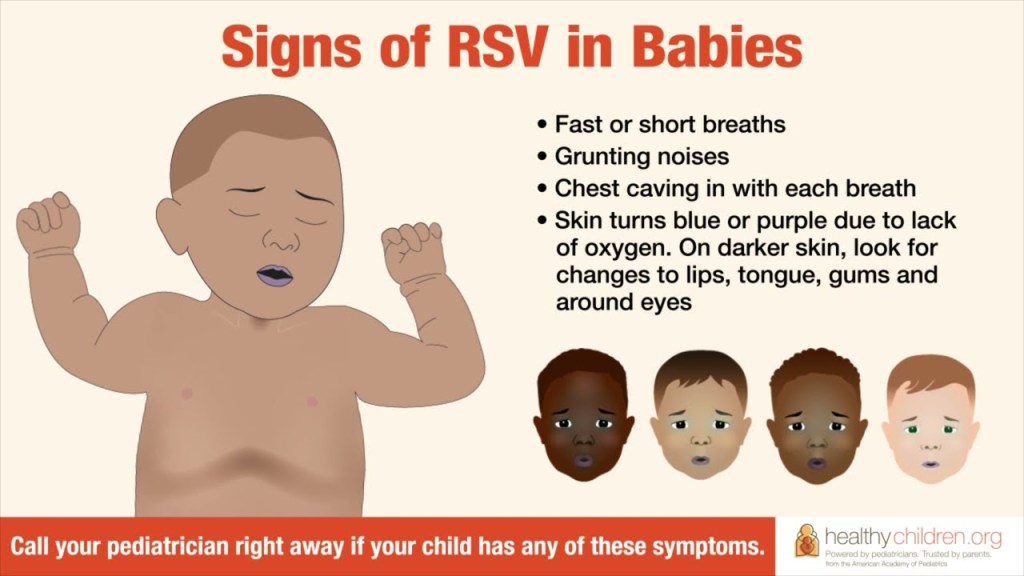
First though, what is RSV?

Respiratory syncytial (sin-Sish-uhl) virus, or RSV, is common respiratory virus which is generally mild but can be very dangerous for infants and the elderly. It typically causes mild, cold-like symptoms. RSV can be serious and is one of the top reasons for hospital admissions in the Fall and Winter for infants.
There are steps you can take to protect your baby, including:
“Conclusion: Breastfeeding has been shown to have a protective effect for infants with RSV bronchiolitis. WHO recommends minimum 6 months of exclusive breastfeeding for maximal immune protection against viral infections in infants.”
Minerva, G. & Phillip, R. 2022. Impact of Breastfeeding on the Incidence and Severity of RSV Bronchiolitis in Infants: Systematic Review. Pediatrics
To learn more check out this article from the CDC.

It can be confusing to figure out because some symptoms of food allergies/intolerance are also found with other types of feeding problems.
So how do you know for sure if your baby has an allergy?
Some symptoms are clearly associated with allergies and intolerance, not just a feeding problem. Babies will generally have more than one of these symptoms.
Food allergies mostly start after baby has started solids in addition to your milk.
While food intolerances, can start at any time. Dairy is the most common in infants.
You only need to remove it from your diet for about 3 days to see a difference. You do need to remove all milk products though. Check this list so you can spot the dairy in the ingredients list.
Other symptoms can go along with food allergies and intolerance but they can also be a sign of another feeding problem.
Colic or discomfort
Poor night time sleep
Not napping
Fussiness after feeds
Temporary green stool
Spit up or reflux
Gassiness
Blood in stool when you have nipple damage
How do you figure out the difference?
Schedule a consult with your IBCLC and they can do a full feeding assessment then refer you to a dietitian and an allergy specialist if a food allergy or intolerance is suspected.
❤ Megan






❤ Megan